Bacterial vaginosis: symptoms, treatment, and prevention
Bacterial vaginosis (BV) is a common vaginal condition caused by an imbalance of bacteria. It often causes a thin gray or white discharge, a fishy smell especially after sex, and sometimes mild burning or itching. Some people have no symptoms. If you notice these signs, a simple check with your clinician can confirm BV and rule out other infections.
Diagnosis usually involves a short exam and either a wet mount microscope test, a pH check of vaginal fluid, or a lab culture. These tests let your provider tell BV apart from yeast or sexually transmitted infections. Tell your clinician about recent antibiotics, douching, new partners, or changes in sexual activity — those details help figure out causes and reduce the chance of repeat episodes.
Treatment options
Standard treatment is a short course of antibiotics. Metronidazole is commonly used either as an oral pill or a vaginal gel. Clindamycin cream is another effective topical choice. Finish the full course even if symptoms improve quickly. If you are pregnant, tell your provider before taking medications — they will pick the safest option for you and your baby.
Recurrence is common: many people have another episode within months. If BV returns, your clinician may prescribe a longer antibiotic course or a different medication. In recurring cases, some providers suggest suppressive therapy with periodic topical antibiotics or partner treatment in specific situations, but partner treatment is not routine.
Prevention and self-care
Avoid douching and scented vaginal products — they disrupt the natural bacterial balance. Use condoms and limit the number of new sexual partners to reduce risk. Wearing breathable cotton underwear and avoiding tight synthetic fabrics can help keep the area dry and less hospitable to bacterial overgrowth. Keeping a record of episodes, triggers, and treatments helps you and your clinician spot patterns.
Some people try probiotics containing Lactobacillus species to restore healthy vaginal bacteria. Evidence is mixed but promising: certain studies show reduced recurrence when probiotics are used alongside or after antibiotics. Talk with your clinician before starting probiotics, especially if you have other health issues.
If you have unusual discharge, strong odor, fever, pelvic pain, or are pregnant with symptoms, see a clinician quickly. Untreated BV can increase the risk of other infections and complications in pregnancy. A prompt check keeps treatment simple and reduces the chance of complications.
Keep communication open with your clinician, follow treatment directions, and note what helps or triggers flare-ups. With the right care and simple lifestyle changes, most people manage BV successfully and reduce repeat episodes.
Over-the-counter home remedies often promise quick fixes, but many lack proof. Avoid douching or using harsh cleansers advertised for odor control. Consider scheduling a follow-up test four weeks after treatment ends if symptoms return. If your clinician prescribes a repeat or suppressive plan, ask about side effects and interactions with other medicines. If you're confused by symptoms or treatments, get a second opinion — a quick consult can save months of repeat problems. Soon.
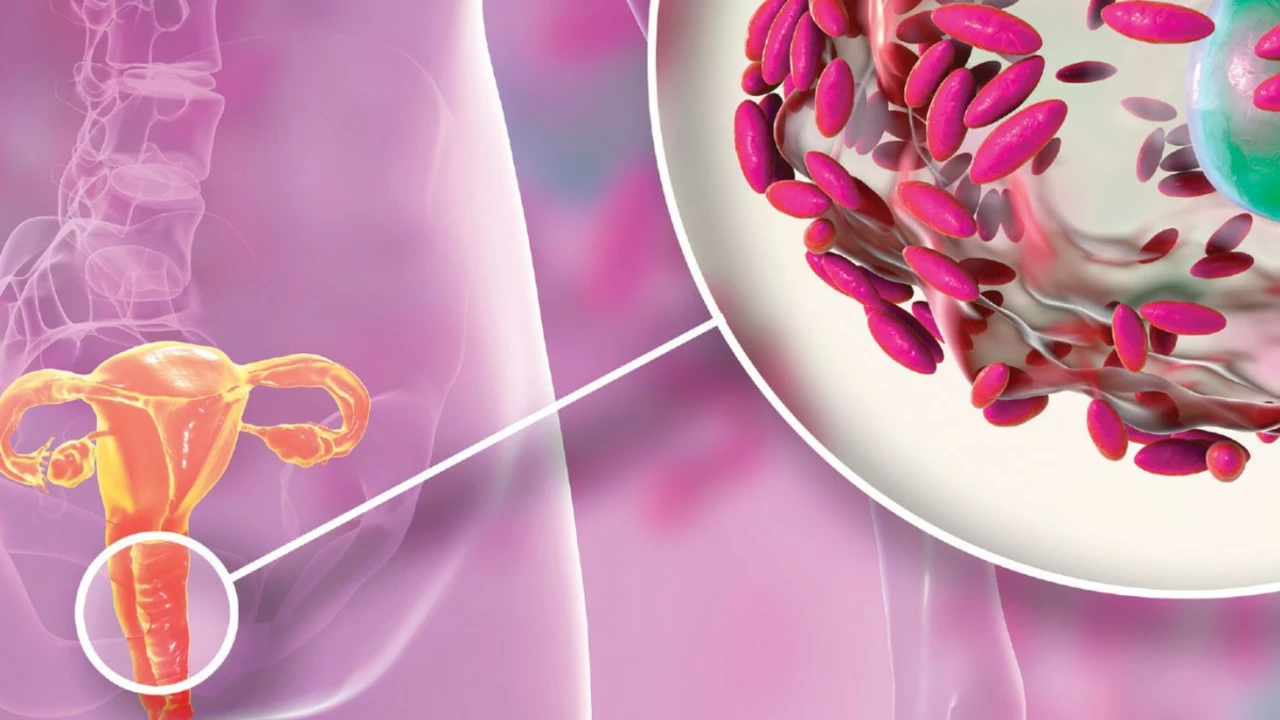
The Role of Chlamydia in Bacterial Vaginosis
Alright, hold on to your hats, folks, because we're about to dive into the wild world of bacteria, specifically Chlamydia and bacterial vaginosis! It's fascinating, really, how the little critters we can't see play such a big part in our lives. Now, Chlamydia, that cheeky little bugger, has quite a role in bacterial vaginosis. It's like the puppet master pulling the strings and causing all sorts of imbalance in the vaginal ecosystem. So, let's give a big hand to our tiny, invisible friends (or should I say foes?) for making life just a tad more interesting!
Detail



