Fungal infection: how to spot, treat, and stop them
Fungal infections are common and usually easy to handle if you act early. You can get them on skin, nails, or in moist places like the groin and mouth. Typical signs include itching, redness, flaky skin, or discolored nails. Knowing what to watch for helps you pick the right treatment and avoid slow, frustrating recurrences.
Common types and what they look like
A few types show up most often. Athlete's foot (tinea pedis) causes itching, burning and peeling between toes. Ringworm (tinea corporis) looks like round, red, scaly patches with clearer centers. Jock itch (tinea cruris) shows up in the groin with redness and itching. Yeast infections affect moist areas—vaginal yeast causes thick white discharge and soreness; oral thrush gives white patches in the mouth. Nail fungus (onychomycosis) makes nails thick, yellow, or crumbly and usually needs longer treatment.
Risk factors raise the chance of fungal infection: sweaty feet, tight shoes, shared locker rooms, antibiotics that upset normal germs, diabetes, and a weak immune system. If you have one of these, act fast when symptoms start.
Practical treatment and prevention tips
For skin infections, start with over-the-counter antifungal creams like clotrimazole, miconazole, or terbinafine. Apply exactly as the label says and keep using for the full course; stopping early is why they come back. Athlete's foot and jock itch often clear in 1–4 weeks with proper use. Nail fungus usually needs prescription treatment and can take months to improve—topical options exist, but many cases need oral medication from a doctor.
If redness spreads fast, you have fever, severe pain, signs of bacterial infection (pus, warmth), uncontrolled diabetes, or you’re immunocompromised, see a clinician right away. Also see a doctor if OTC medicine doesn’t help after the recommended time or if the infection keeps returning.
Prevention is simple: keep affected areas clean and dry, change socks daily, wear breathable shoes, and avoid walking barefoot in public showers. Don’t share towels, shoes, or nail tools. For athletes or frequent gym users, use a powder or antifungal spray in shoes. If you take antibiotics often, chat with your doctor about ways to protect your natural balance of germs.
Quick note on home remedies: some people try tea tree oil or vinegar. These can help mildly but aren’t as reliable as tested antifungals. Don’t use harsh chemicals or unproven DIY mixes on broken skin. When in doubt, get a simple exam—sometimes a swab or nail clipping confirms the fungus and speeds up the right treatment.
Fungal infections are usually manageable. Spot them early, follow treatment directions, and take basic prevention steps to stop them from coming back.
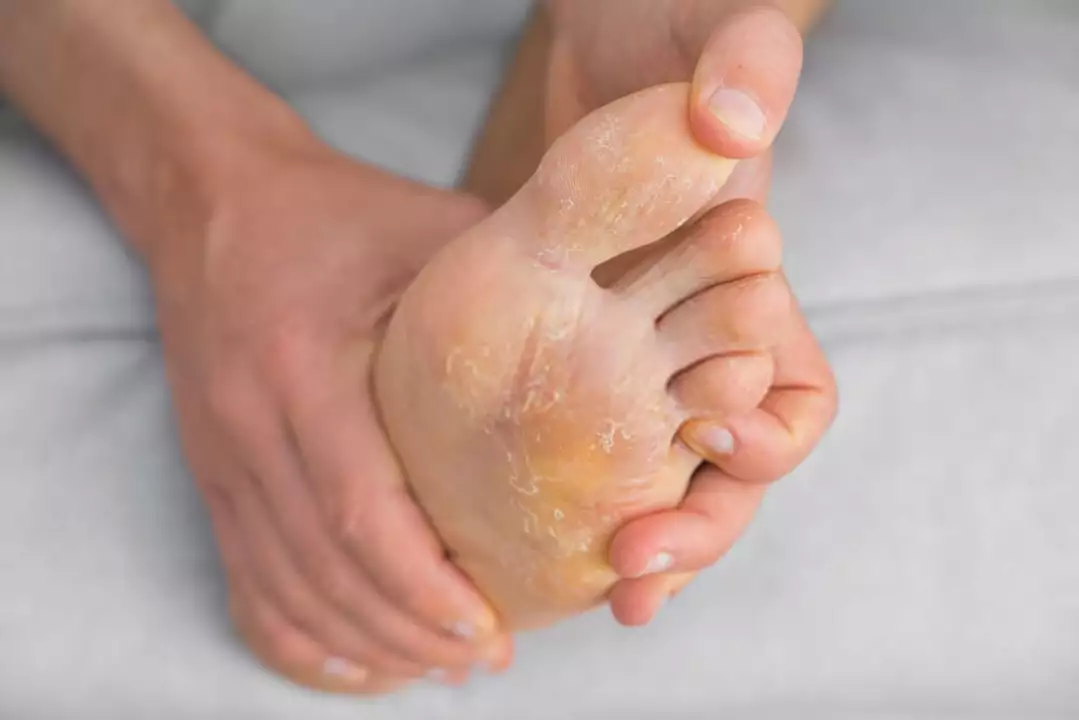
The Surprising Link Between Athlete's Foot and Stress
In a recent blog post, I explored the surprising connection between athlete's foot and stress. It turns out that stress can weaken our immune system, making us more susceptible to fungal infections like athlete's foot. Additionally, stress can exacerbate existing infections, leading to more severe symptoms. To prevent this uncomfortable condition, it's essential to manage stress through relaxation techniques and self-care. So, next time you're feeling stressed, remember to take a step back and prioritize your well-being to keep your feet healthy and fungus-free.
Detail